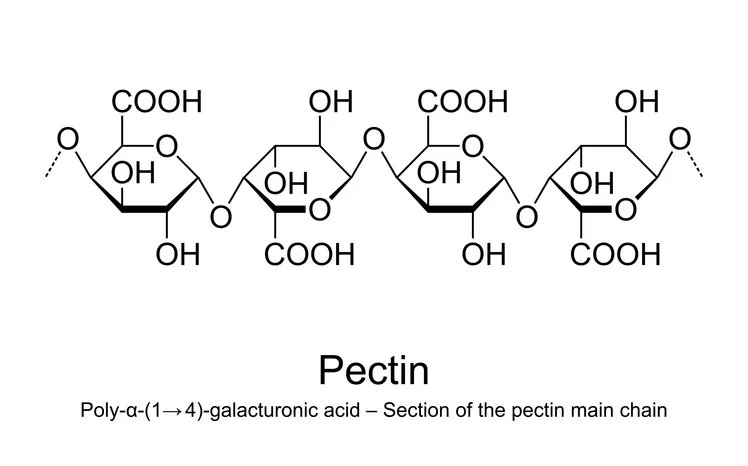
Debunking Fiber: From Health Staple to Hidden Hindrance
For decades, health authorities have pushed dietary fiber as an indispensable part of a balanced diet. We're told it prevents constipation, lowers cholesterol, regulates blood sugar, and even wards off diseases like heart disease and cancer. Guidelines from organizations like the American Heart Association and Mayo Clinic recommend 25-30 grams daily, often citing studies linking high-fiber intakes to better health outcomes. But what if this is a fallacy? What if fiber isn't essential and, for many people, acts more like an antinutrient—something that hinders rather than helps? Let's dissect this myth, drawing on evidence from nutrition science, evolutionary biology, and real-world dietary experiments.
First, understand what fiber is: indigestible plant material, such as cellulose, lignin, and pectin, that humans lack the enzymes to break down. Unlike proteins, fats, or carbohydrates, fiber passes largely unchanged through the digestive system. Proponents argue it adds bulk to stool, promotes satiety, and feeds gut bacteria, producing beneficial short-chain fatty acids (SCFAs) that support immunity and reduce inflammation. Yet, the absence of a fiber deficiency state in humans tells a different story. There's no established Recommended Dietary Allowance (RDA) for fiber because no deficiency symptoms arise without it—unlike true essential nutrients like vitamin C or iron, this alone questions its "essential" status.
The fallacy begins with the assumption that fiber is universally beneficial. Observational studies often show that high-fiber diets are associated with lower risks of obesity, diabetes, and cardiovascular disease. However, these studies are plagued by confounders: people who eat more fiber-rich foods (fruits, vegetables, whole grains) often lead healthier lifestyles overall, exercising more, and avoiding processed junk. When isolated, fiber's benefits diminish. A comprehensive review in the World Journal of Gastroenterology found no strong evidence that fiber protects against colorectal cancer or polyps. Similarly, claims that fiber prevents constipation are overstated. One study showed that reducing or eliminating fiber actually improved constipation symptoms, challenging the "broom for the gut" analogy.
Now, consider fiber's role as an antinutrient. Antinutrients are compounds in plants that can interfere with nutrient absorption, and fiber fits this bill. Soluble fibers, such as pectin, bind to minerals like calcium, iron, and zinc, reducing their bioavailability. Insoluble fibers add bulk but can irritate the intestinal lining, leading to inflammation, bloating, and gas—symptoms familiar to those with IBS or Crohn's disease. In fact, fiber fermentation in the colon produces gases such as hydrogen and methane, which can cause discomfort rather than relief. For many, especially those with sensitive guts, fiber can feel like sandpaper, eroding the mucosal lining and exacerbating dysbiosis (an imbalance of gut bacteria).
Evolutionary perspectives bolster this view. Humans aren't ruminants like cows, with multi-chambered stomachs designed to ferment plant fiber. Our ancestors thrived on animal-based diets during the ice ages, when plants were scarce. The human stomach's low pH (around 1.5) is more akin to that of carnivores and scavengers, optimized for breaking down meat rather than cellulose. Modern hunter-gatherers like the Hadza consume fiber seasonally but don't rely on it year-round, suggesting that fiber tolerance varies: for some, it's neutral or beneficial, but for others—particularly those with modern gut issues—it's problematic.
Enter the carnivore diet, a zero-fiber approach that's gained traction for resolving digestive woes. Advocates report fewer bowel movements (due to less waste), no constipation, and improved energy, as the body absorbs nearly all nutrients from animal foods without interference. A study on carnivore adherents found benefits for chronic conditions, despite fiber intake being "significantly below recommended levels." Critics warn of microbiome disruption, but emerging research shows that gut bacteria adapt and thrive on animal-derived substrates, such as mucin. One X post highlights "hidden fiber" in meat that feeds bacteria without plant bulk.
Fiber can also spike insulin and glucose less than carbs alone, acting as an "anti-carb" by slowing absorption. But this benefit is double-edged: it may mask underlying carb intolerance while causing long-term gut irritation. For diabetics or those with metabolic syndrome, removing fiber (and carbs) often stabilizes blood sugar better. Moreover, high-fiber diets can lead to nutrient deficiencies in vulnerable groups, such as children and the elderly, by binding essential minerals.
Not everyone reacts poorly to fiber—genetics, microbiome composition, and overall diet play roles. Some thrive on high-fiber plant-based eating, with studies showing reduced CVD risk. But for the millions suffering from IBS (affecting 10-15% of people), low-fiber or zero-fiber diets offer relief where traditional advice fails. The key is personalization: if fiber causes bloating or irregularity, it's not your friend.
In conclusion, the fiber fallacy stems from oversimplified correlations and industry influence (think cereal companies promoting bran). While it may benefit some, labeling it "essential" ignores its potential as an antinutrient and the success of low-fiber diets. Listen to your body—if ditching fiber resolves issues, that's evidence enough. Consult a professional before major changes, but question the dogma. Health isn't one-size-fits-all; sometimes, less bulk means more vitality.